Female urinary incontinence
The intervention is performed on an outpatient basis under local or loco-regional anesthesia. It lasts 15 minutes. The pain is minimal thereafter.
Urethral strip to treat urinary incontinence
Dr. Velemir specializes in the management of female urinary incontinence and closely follows the latest therapeutic developments.
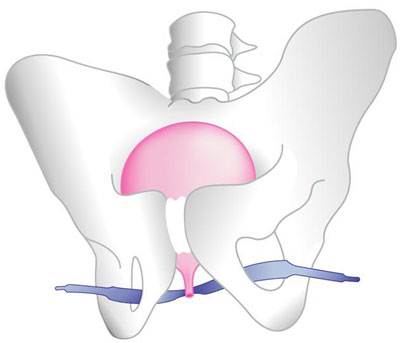
What is female urinary incontinence? How common is it?
Defined as the involuntary loss of urine, urinary incontinence is often regarded by women as a taboo subject, and many women avoid talking about it to their doctor or their relatives.
The frequency of female urinary incontinence increases with age and affects:
Are there several kinds of female urinary incontinence ?
Yes, we must distinguish between:
What treatments are there?
Urge incontinence is first treated by drugs. The goal of treatment is to calm inopportune bladder contractions to reduce the frequency but also the volume of urine leakage throughout the day or night. When medical treatment has failed, urge incontinence can be treated by sacral neuromodulation. This is a technique that involves implanting a small electrode at the bottom of the back. It is connected to a small portable device that will help regulate the electrical signal controlling the contraction of the bladder.
Stress incontinence is treated first by rehabilitation of the perineum and in cases where the results are unsatisfactory, it can be treated with surgery.
What kind of surgery is used to treat incontinence?
Many techniques exist, but urethral support slings, which have existed since 1996, have revolutionised the treatment of urge urinary incontinence. These slings have been modified in different ways, and this has led to a variety of names: TVT, TOT, Mini slings.
In urinary incontinence, it is the lack of support under the urethra (the small canal through which urine exits the bladder during urination) during any kind of physical effort that leads to urine leakage. The operation involves placing a synthetic sling under the urethra. This sling forms a solid hammock. When there is any kind of extra physical effort, the urethra hits the sling and closes, preventing urine leakage. To fully understand the anti-leakage mechanism of the sling, you can imagine a garden hose open and placed on the grass. If you press it with your foot to stop the water flow, the hose sinks into the grass and the water continues to flow. If the hose is placed on a solid plane like concrete, and you press it with your foot, then the hose is squeezed, and the water stops flowing.
What does this intervention consist of?
The procedure is performed on an outpatient basis under local or loco-regional anaesthesia. It lasts 15 minutes. The pain is minimal thereafter. In the hours after the intervention, the patient is asked to drink a lot of fluid and then to urinate. The post-void residual in the bladder is then measured by a catheter for voiding. It should be low, which means that the patient can empty her bladder well and that the sling is not too tight. The patient can then go home.
The sling usually takes one month to integrate with tissues and provide an effective supporting role. During this healing period, it is essential that the patient rests, avoids major effort such as carrying heavy loads, otherwise the sling could loosen itself and the final result would not be assured.
What is the success rate of this intervention?
It is of 90% at 1 year. This result remains stable over time with a cure rate of 85% at 10 years.
Should we pass additional tests before the operation?
A urodynamic evaluation and urine tests are performed in preparation for the operation.
What is a urodynamic evaluation?
This is a simple and painless test that allows us to better understand how the bladder and the muscles that control urination (the action to urinate) work. It enables us to refine the analysis of any disorders and to better adapt treatment. The examination is performed in Dr Velemir’s office.